Join the Leading Global Eye Health Alliance.
MembershipIntegrated people-centred eye care (IPEC) has the potential to address many challenges to delivering effective eye care services.
Integrated people-centred eye care (IPEC):
The implementation of integrated people-centred eye care requires four strategies to ensure people get the right care, at the right time, in the right place.
Select the arrows below to learn more.
In IPEC, services must be coordinated across the different levels and sites of care within and beyond the health sector.
IPEC builds upon and extends previous strategic plans for eye health system development, that promoted integrating eye health with health and non-health sectors and strengthening of primary eye-care services.
The following diagram is based on figure 17 in The Lancet Global Health Commission on Global Eye Health (Burton et al., 2021).
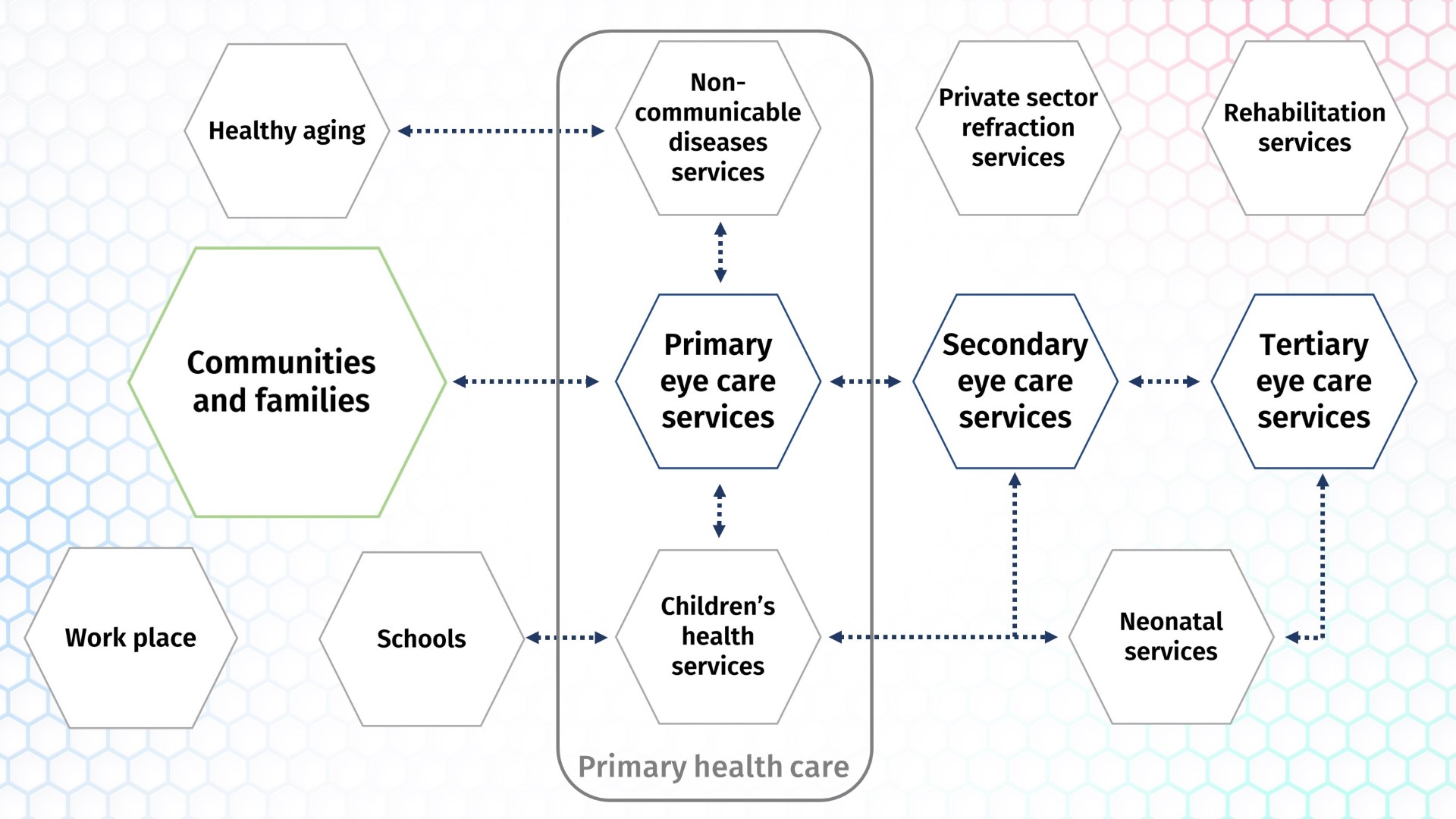
IPEC aims for improved service delivery, care experiences and outcomes.
People should be empowered as effective users and beneficiaries of eye health services. This should continue throughout all stages of their lives and as their health needs change.
Select each tab below to learn more about person-centred eye care services.

When implementing IPEC, primary eye care must be included in primary health care. An example is eye care training for nurses in local medical clinics.
Primary eye care is needed in all countries as it connects eye health with the wider primary health system.
Primary care staff such as doctors and nurses need to identify eye health problems and refer patients to specialized eye care services when required.
Sustained leadership and governance are required in IPEC to develop a strategic plan based on the current situation in eye care in a country, manage accountability and oversee the plan’s implementation.
Eye care planning should be led by the national eye health committee or working group, who will lead and provide technical input for IPEC.