Join the Leading Global Eye Health Alliance.
Membership-
Choose an alternate language here
- Membership
[vc_row][vc_column][vc_column_text]For World Glaucoma Week, Dr Scott Lawrence, Kellogg Eye Center for International Ophthalmology (KECIO) at the University of Michigan, writes about the three “As” of Glaucoma care in Africa.
I had recently moved from my comfortable academic practice in the United States to work full-time in Ethiopia when SG, a 45-year-old mother of three young children, pushed her way into my exam room. She had just received news that she was rapidly losing vision from glaucoma and that it was probably too late to save her sight. Her 400-kilometre journey to see me did not diminish her determination.
“I don’t want to go blind! My children need me,” she exclaimed. Medications had done little to control her eye pressures. I held up her 10-degree visual field printouts: any observer could easily see that she had been reduced to “tunnel vision”. After a long discussion, I scheduled her for surgery.

Like SG, approximately 90% of people with glaucoma in Africa lack awareness that they have the disease. It is as if their sight has been secretly stolen. Of those who have been identified, many have poor understanding of glaucoma, thinking their condition is reversible or not related to their vision loss. They are less prone to persist with medical treatment and more likely to refuse surgery. Counseling services and educational materials can help these patients process their diagnosis. Public service announcements and campaigns can spring communities into action.
In my experience, patients often harbour distrust of the health system because of unfamiliarity or a bad experience. Adherence may be undermined by traditional beliefs or a sense of fatalism. Topical medications, a mainstay of therapy in much of the world, are relatively expensive or unavailable on local markets. As physicians, we must communicate with patients, addressing their concerns and beliefs. It is important that we teach our patients and their families about glaucoma and train them how to administer their medications. Investing in systems by developing supply lines, marketing, variable pricing, and distribution of pharmaceuticals is a major need in Africa.
A third, and possibly the most significant, barrier to managing glaucoma in Africa is access. SG, with the help of extended family who paid for her transportation, was able to receive sight-saving surgery, but many patients are not so fortunate.
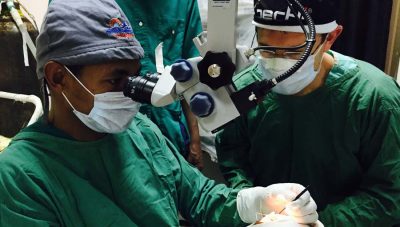
From my perspective, high-level training of ophthalmology residents and glaucoma subspecialists is the most important and sustainable contribution we can make to alleviate blindness from glaucoma in Africa. Having successfully expanded the number of ophthalmology training programmes, emphasis is turning to the need for strong subspecialty training opportunities. Through a recent collaboration between charitable organizations, industry leaders, and the Kellogg Eye Center for International Ophthalmology (KECIO) at the University of Michigan, we have launched a glaucoma fellowship training programme at St. Paul’s Hospital Millennium Medical College in Addis Ababa. Similar efforts are underway at other institutions as well. We hope that initiatives like these throughout Africa will perpetuate a skilled work force that is equipped to address glaucoma and save sight for years to come.[/vc_column_text][/vc_column][/vc_row][vc_row el_class=”light-row rebelcell prev-blind”][vc_column width=”1/2″ el_class=”cellspace”][vc_column_text]
[/vc_column_text][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_row_inner][vc_column_inner][vc_column_text]
[/vc_column_text][/vc_column_inner][/vc_row_inner][vc_separator color=”white”][vc_row_inner][vc_column_inner][vc_column_text]
[/vc_column_text][/vc_column_inner][/vc_row_inner][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_row_inner][vc_column_inner][vc_column_text]
[/vc_column_text][/vc_column_inner][/vc_row_inner][vc_separator][/vc_column][vc_column width=”1/2″ el_class=”cellspace”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_row_inner][vc_column_inner][vc_column_text]
[/vc_column_text][/vc_column_inner][/vc_row_inner][vc_separator color=”white”][vc_row_inner][vc_column_inner][vc_column_text]
[/vc_column_text][/vc_column_inner][/vc_row_inner][vc_separator color=”white”][vc_row_inner][vc_column_inner][vc_column_text]
[/vc_column_text][/vc_column_inner][/vc_row_inner][vc_separator color=”white”][vc_row_inner][vc_column_inner][vc_column_text]
[/vc_column_text][/vc_column_inner][/vc_row_inner][vc_separator color=”white”][vc_row_inner][vc_column_inner][vc_column_text]
[/vc_column_text][/vc_column_inner][/vc_row_inner][/vc_column][/vc_row]