Join the Leading Global Eye Health Alliance.
Membership-
Choose an alternate language here
- Membership
For World Glaucoma Week, Dr Marvice Okwen on glaucoma in Cameroon and what needs to be done…
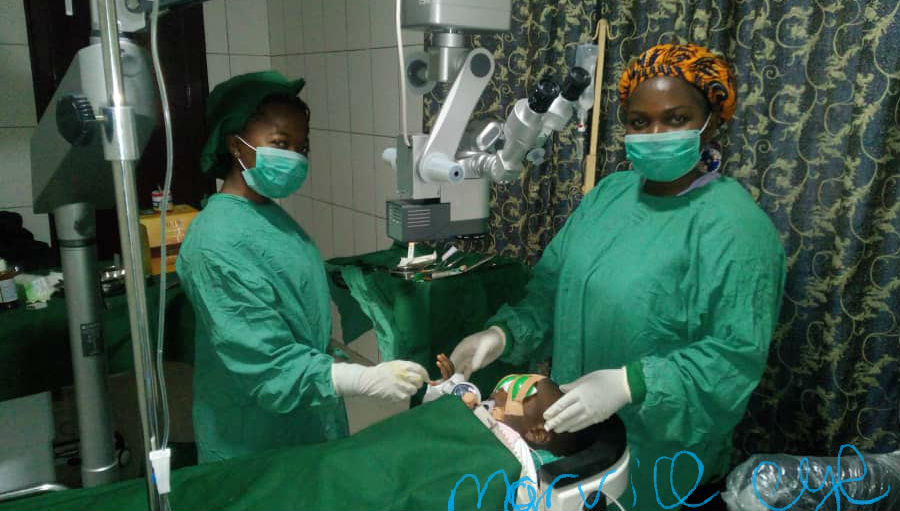 While setting up my slit lamp, a blind man walked in, holding a 2month old baby; and said, ‘doctor! I heard you over the radio talking about glaucoma in children; I think my child has the kind of eyes you described! Big, grey, blinking and tearing excessively especially on exposure to light! I’m blind because of parental ignorance, both eyes plugged off due to pain; I’m now knowledgeable and won’t let it happen to anyone. My daughter will be my sight even though I am blind’
While setting up my slit lamp, a blind man walked in, holding a 2month old baby; and said, ‘doctor! I heard you over the radio talking about glaucoma in children; I think my child has the kind of eyes you described! Big, grey, blinking and tearing excessively especially on exposure to light! I’m blind because of parental ignorance, both eyes plugged off due to pain; I’m now knowledgeable and won’t let it happen to anyone. My daughter will be my sight even though I am blind’
After evaluation under anesthesia, primary congenital glaucoma was confirmed. She had a successful surgery and today she is 5years old with clear corneas, normal pressures and a visual acuity of 6/6 in both eyes and doing great in school.
In Cameroon, prevalence of blindness is about 0.5% 1,2, Glaucoma being the second most common cause. (19.7%) and 3rd leading cause in children(10%)2.
Factors accounting for poor prognosis of congenital glaucoma in Cameroon include:
ABII Foundation, Bamenda, is setting up a system that takes into consideration these challenges to facilitate early diagnosis, affordable care through a community-based approach. Azah regained her sight because her father was made aware of the symptoms of glaucoma and she presented early.
Unfortunately, we see many children presenting late and that usually results in poor outcomes even after surgery.
Sensitization through active participation of village and religious heads, midwives, ANC nurses, and teachers who are often the ‘first contact’ will lead to early recognition and referral. Behavioral changes and support groups. We need to know the importance of routine eye checkups even in the absence of symptoms. The government needs better reconstruction of hospitals and needs to equip them (ophthalmoscopes, Perimeters, OCT, lasers, tonometers, etc.) to be able to address early years ophthalmic conditions and ensure easy access to these services.
An organized referral system, Human resource development, task shifting with enhanced supervision has proven useful (4).
Eye care inclusion in basic education curriculum, support to community and school outreach eye care programmes are important.
Sensitization, early diagnosis and treatment with routine eye check up, for all from birth will avoid Glaucoma stealing our sight silently and turning our light into darkness!
Reference
1.prevalence of visual impairment in Fundong DISTRICT
OYE J, Mactaggart I,Schmidt, E, Tamo V, Okwen M,, Sept 2017, Ophthalmic Epidemiology
2.Andre O et al, ‘prevalence and causes of blindness at a tertiary hospital in Douala, Cameroon, Sept. 2011 clinical ophthalmology 5910:1325-31
3.Okwen m, Signe R, Macpella sm, mbibeh L, Cockburn L. professional collaboration for vision and healthcare in Cameroon. Afr vision Eye health. 2018;77?(1), a 434. https://doi.org/10.4102/aveh.v77i1.434
4.Okwen M, et al., Primary eye care skills scores for health workers in routine and enhanced supervision settings, Public Health (2013), http://dx.doi.org/10.1016/j.puhe.2013.10.007
[vc_row_inner css=”.vc_custom_1583749525922{background-color: #e7ecf3 !important;}”][vc_column_inner width=”1/2″ css=”.vc_custom_1583749682211{padding-left: 15px !important;}”]
[vc_column_text]
The IAPB Global Assembly 2020 (GA2020) programme has several sessions on Glaucoma. If your work is around the topic, do submit an abstract–the sector needs to know!
[/vc_column_text][/vc_column_inner][vc_column_inner width=”1/2″][vc_single_image image=”88500″ img_size=”400×263″][/vc_column_inner][/vc_row_inner][vc_row][vc_column][vc_column_text][/vc_column_text][/vc_row]
[vc_row el_class=”light-row rebelcell prev-blind”][vc_column width=”1/2″ el_class=”cellspace”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][/vc_column][vc_column width=”1/2″ el_class=”cellspace”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][vc_column_text]
[/vc_column_text][vc_separator color=”white”][/vc_column][/vc_row]